Experience Design
From complex problem spaces to elegant experiences, I design alongside my teams in braiding together the strategy, research, design systems, and product thinking to all work together.

UnitedHealthcare Medicare Shopping / Online Enrollment
Primary challenges to solve for:
A higher level of enrollments
Each piece is made with attention to detail, ensuring quality you can trust and a finish you’ll be proud to show off.
01
Simplify the experience to reduce drop off rates
From texture to tone, we consider the small things—because they’re what make a product truly stand out.
02
Enable users with an increased sense of confidence
Our products aren’t just nice to look at—they’re built to integrate into your life with ease, purpose, and durability.
03
Challenge
UnitedHealthcare’s Online Enrollment experience for Medicare Advantage plans was seeing strong traffic but declining performance where it mattered most: application completion.
While overall enrollment starts were increasing year over year, the start-to-completion rate had dropped, particularly among users on mobile devices. At the same time, the audience using the tool was expanding to include a wider range of demographics with different needs and levels of technical comfort.
Several issues were contributing to friction:
A complex, high-stakes process
Applying for Medicare coverage requires users to provide detailed personal, medical, and eligibility information. Many users were unfamiliar with the process and uncertain about what information they would need.
Lack of clarity and confidence during the application flow
User testing revealed participants often didn’t know where they were in the process or how much work remained. This uncertainty led to hesitation and abandonment.
Fragmented interaction patterns
The enrollment flow had evolved over time using older design systems and inconsistent UI patterns, which created a disjointed experience across steps.
Mobile usability gaps
Traffic from mobile devices had increased significantly, but the experience had not been optimized for smaller screens or touch interactions.
Diverse user scenarios
Personas ranged from newly eligible individuals turning 65 to caregivers applying on behalf of family members, as well as existing members comparing plans or switching coverage. Each group approached enrollment with different levels of knowledge and confidence.
My UX team’s goal was to increase enrollment completion rates while improving clarity, usability, and trust throughout the application journey.
Approach
To address these issues, the team redesigned the enrollment experience around three guiding principles: clarity, confidence, and consistency.
Prepare users
Users wanted to prepare before starting so they wouldn’t get stuck mid-application.
01: Grounding the experience in real user needs
“ It’s always helpful when someone gives you a heads-up to get something ready with a little advance notice. ”
Show progress
Participants struggled to understand where they were in the process.
“ I’m not totally sure where I am in it. Maybe about half way through? I didn’t see anything that shows how far along you are.”
Assist users
Small accessibility usability improvements like formatting assistance or contextual help significantly reduced hesitation.
“It would have been easier if the letters were capitalized automatically so I didn’t have to do it myself.”
For example, participants responded positively when the experience explained what documents they would need before starting, such as a Medicare card or insurance details.
These insights shaped design priorities across the entire flow.
02: Re-mapping the end-to-end enrollment journey
Key benefits of the flow redesign included:
Identifying steps where users most commonly abandoned the process
Reducing redundant pages
Clarifying the sequence of required information
Creating alignment between design, product, and engineering teams
The final structure organized the experience into clear stages:
Personal information
Eligibility verification
Contact information
Additional coverage details
Review and submit
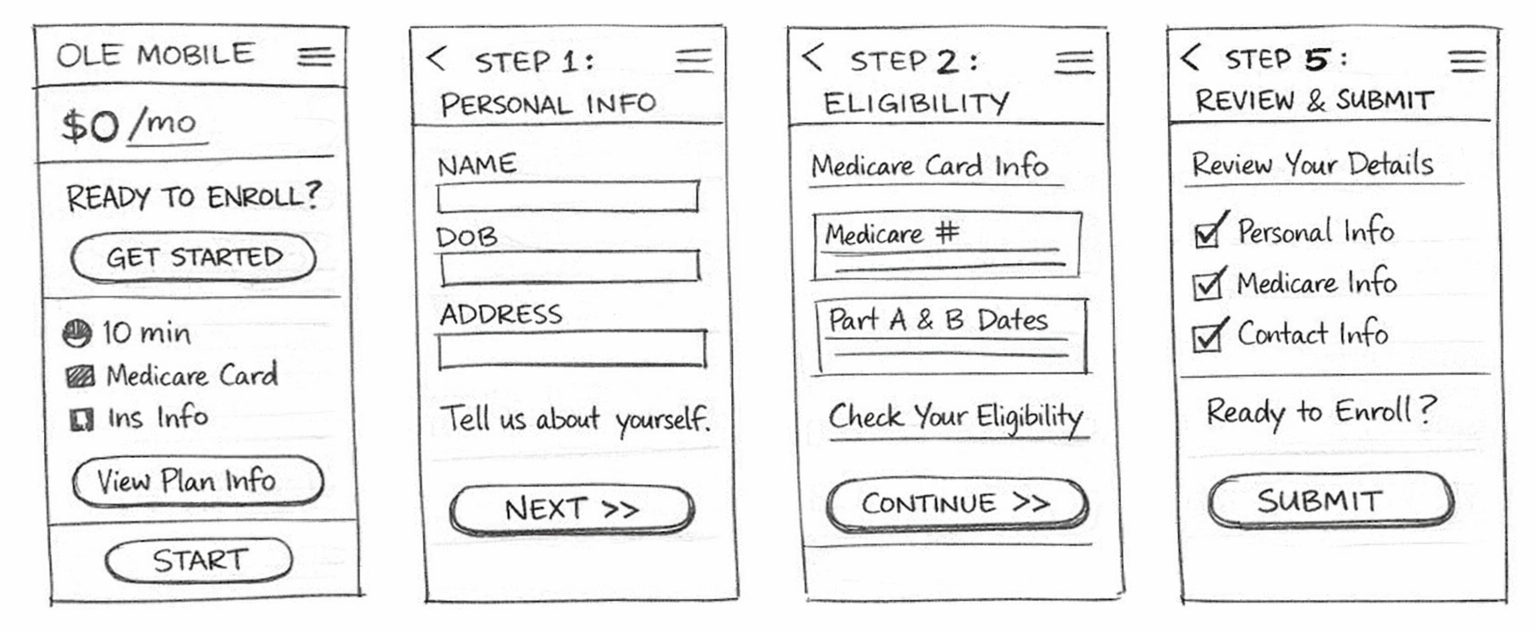
03: Establishing clear page templates
To improve consistency and scalability, the team created a system of reusable page patterns.
These templates defined the structure for the entire application experience:

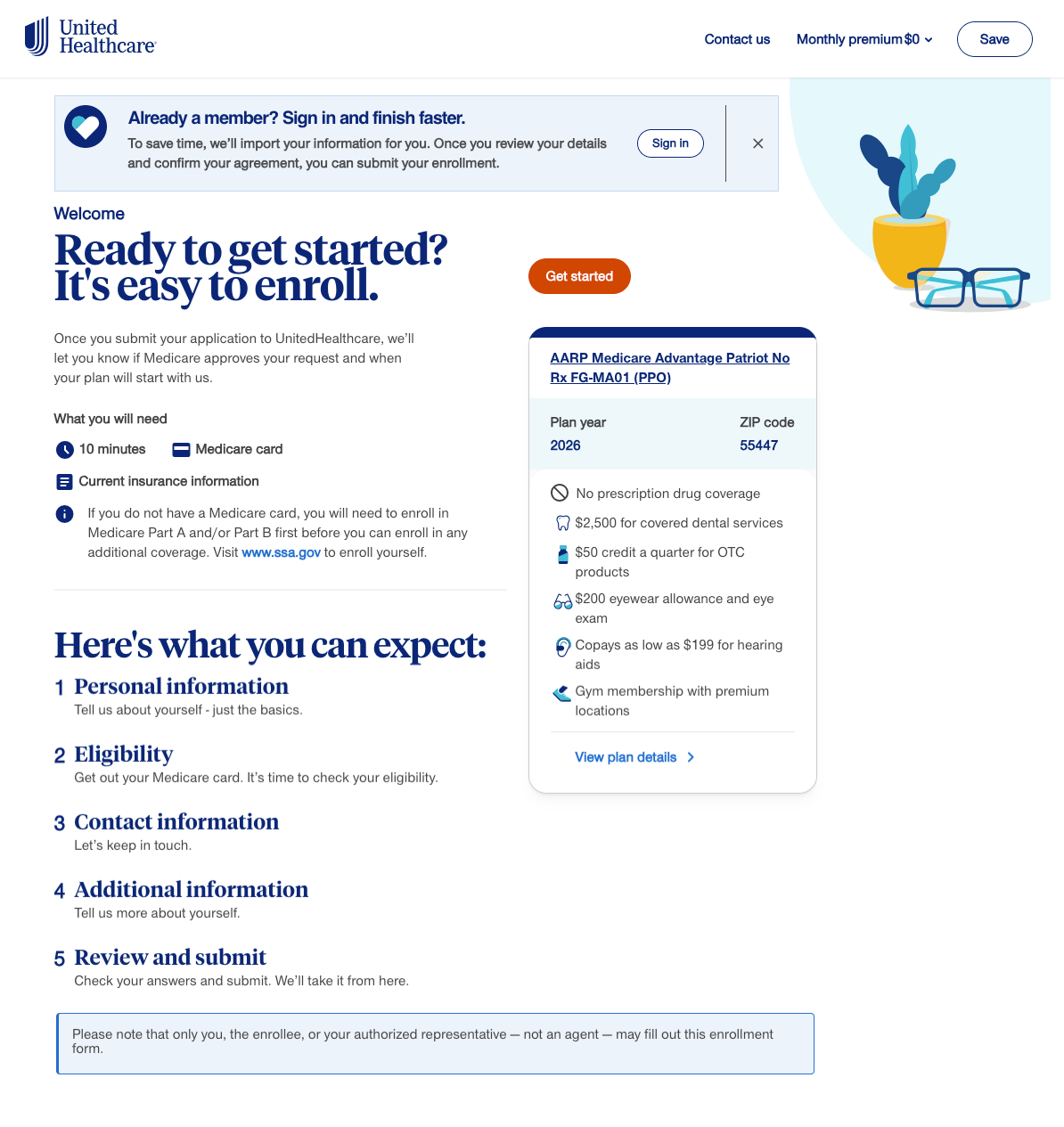
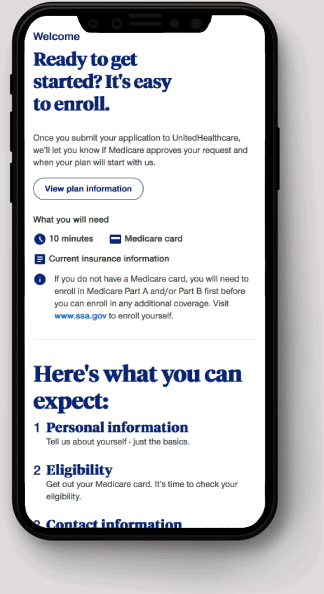
Welcome page / Introduced the process and helped users prepare by outlining what information they would need.

Section landing pages / Signaled the beginning of a new stage and reinforced progress.

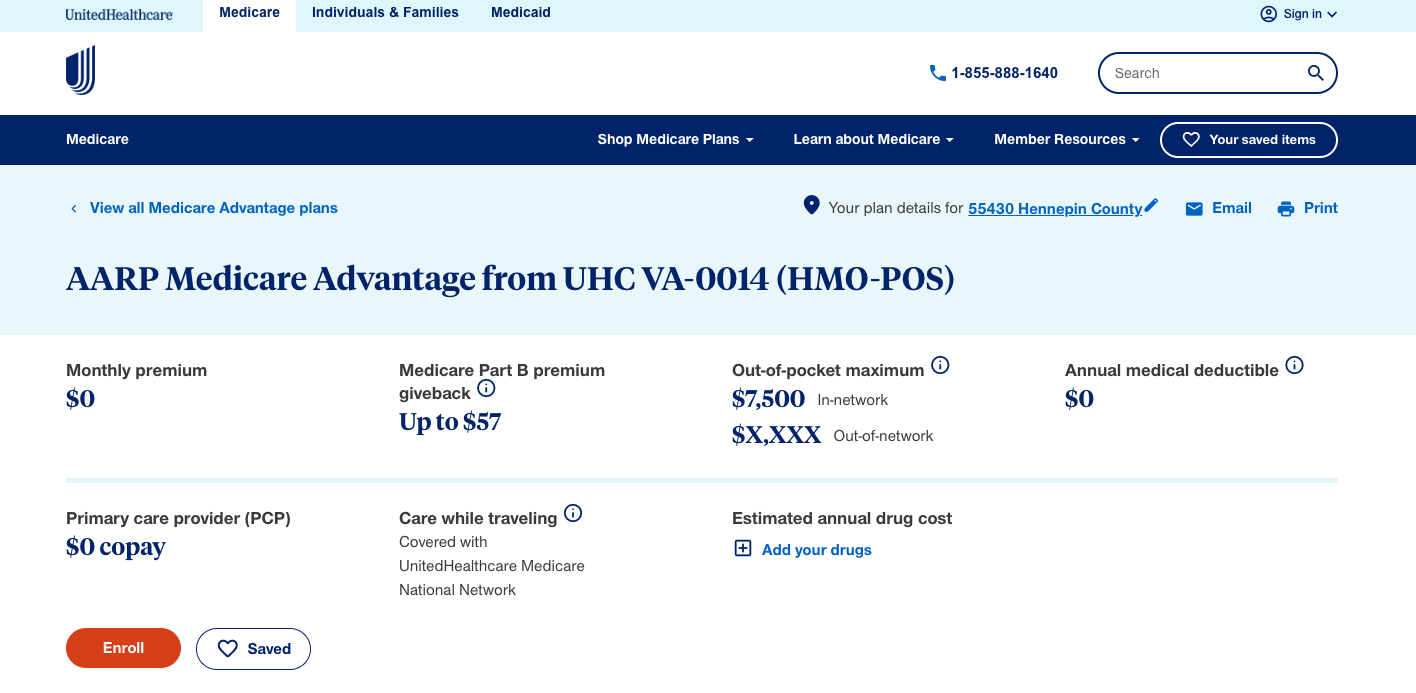
Input pages / Focused, task-oriented screens where users entered or confirmed information.

Review pages / Allowed users to verify their entries before submission.
04: Integrating the design system
To improve consistency and scalability, the team created a system of reusable page patterns.
These templates defined the structure for the entire application experience:
Approach
To address these issues, the team redesigned the enrollment experience around three guiding principles: clarity, confidence, and consistency.
Grounding the experience in real user needs
Research and usability testing revealed several key behavioral insights:
Users wanted to prepare before starting so they wouldn’t get stuck mid-application.
Participants struggled to understand where they were in the process.
Small usability improvements like formatting assistance or contextual help significantly reduced hesitation.
For example, participants responded positively when the experience explained what documents they would need before starting, such as a Medicare card or insurance details.
These insights shaped design priorities across the entire flow.
UnitedHealthcare Medicare Shopping / Online Enrollment
Challenge
UnitedHealthcare’s Online Enrollment (OLE) experience for Medicare Advantage plans was seeing strong traffic but declining performance where it mattered most: application completion.
While overall enrollment starts were increasing year over year, the start-to-completion rate had dropped, particularly among users on mobile devices. At the same time, the audience using the tool was expanding to include a wider range of demographics with different needs and levels of technical comfort.
Several issues were contributing to friction:
1. A complex, high-stakes process
Applying for Medicare coverage requires users to provide detailed personal, medical, and eligibility information. Many users were unfamiliar with the process and uncertain about what information they would need.
2. Lack of clarity and confidence during the application flow
User testing revealed participants often didn’t know where they were in the process or how much work remained. This uncertainty led to hesitation and abandonment.
3. Fragmented interaction patterns
The enrollment flow had evolved over time using older design systems and inconsistent UI patterns, which created a disjointed experience across steps.
4. Mobile usability gaps
Traffic from mobile devices had increased significantly, but the experience had not been optimized for smaller screens or touch interactions.
5. Diverse user scenarios
Personas ranged from newly eligible individuals turning 65 to caregivers applying on behalf of family members, as well as existing members comparing plans or switching coverage. Each group approached enrollment with different levels of knowledge and confidence.
The team’s goal was to increase enrollment completion rates while improving clarity, usability, and trust throughout the application journey.
Approach
To address these issues, the team redesigned the enrollment experience around three guiding principles: clarity, confidence, and consistency.
1. Grounding the experience in real user needs
Research and usability testing revealed several key behavioral insights:
Users wanted to prepare before starting so they wouldn’t get stuck mid-application.
Participants struggled to understand where they were in the process.
Small usability improvements like formatting assistance or contextual help significantly reduced hesitation.
For example, participants responded positively when the experience explained what documents they would need before starting, such as a Medicare card or insurance details.
These insights shaped design priorities across the entire flow.
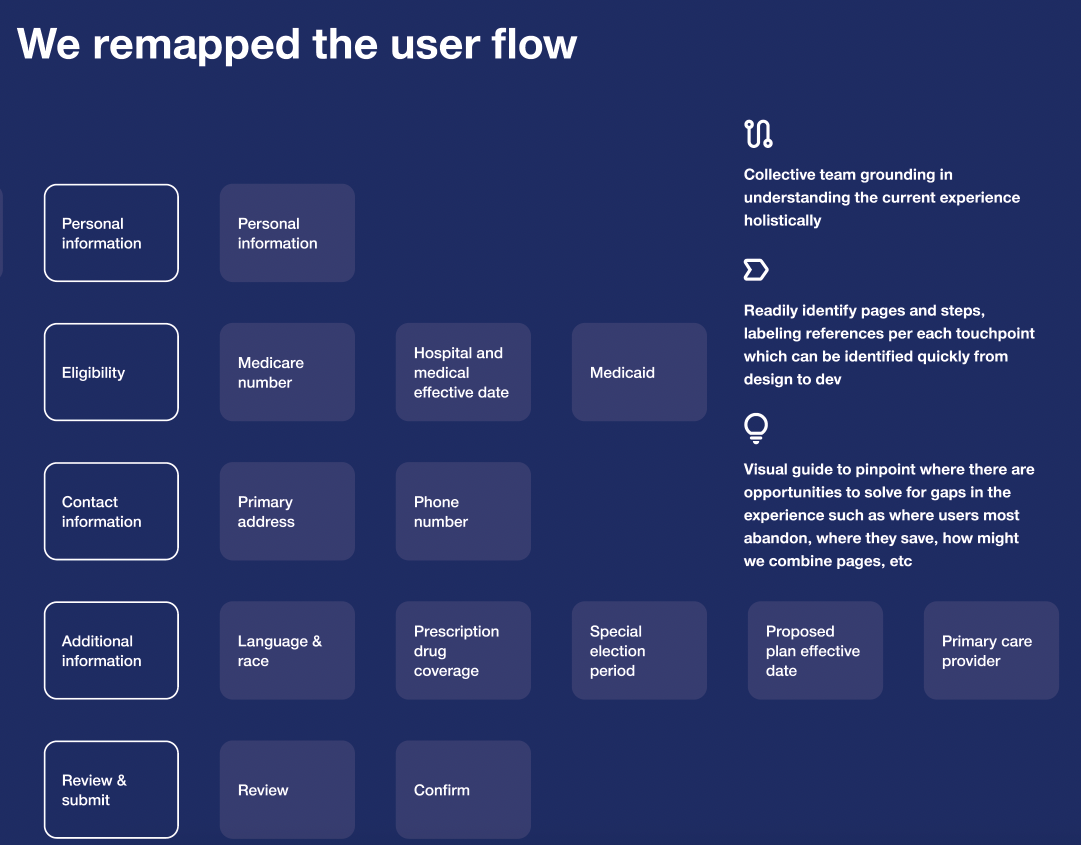
2. Re-mapping the end-to-end enrollment journey
The team conducted a complete audit of the existing enrollment process and remapped the user flow to identify friction points and opportunities to simplify.
Key benefits of the flow redesign included:
Identifying steps where users most commonly abandoned the process
Reducing redundant pages
Clarifying the sequence of required information
Creating alignment between design, product, and engineering teams
The final structure organized the experience into clear stages:
Personal information
Eligibility verification
Contact information
Additional coverage details
Review and submit
This structure helped establish a predictable rhythm that users could follow confidently from start to finish.
3. Establishing clear page templates
To improve consistency and scalability, the team created a system of reusable page patterns.
These templates defined the structure for the entire application experience:
Welcome page
Introduced the process and helped users prepare by outlining what information they would need.
Section landing pages
Signaled the beginning of a new stage and reinforced progress.
Input pages
Focused, task-oriented screens where users entered or confirmed information.
Review pages
Allowed users to verify their entries before submission.
This modular structure ensured users would not have to relearn interactions from screen to screen.
4. Integrating the Abyss design system
The redesign aligned the enrollment experience with the company’s Abyss design system, bringing modern UI components and accessibility improvements into the product.
Design system elements introduced included:
standardized alerts and notifications
improved progress indicators
contextual help popovers
accessible form controls
consistent visual hierarchy
By aligning with the broader system, the experience gained both visual cohesion and engineering efficiency.
5. Increasing transparency and reassurance
Healthcare enrollment can feel intimidating. The redesign intentionally added signals to build user confidence throughout the journey.
Key improvements included:
Progress visibility
A persistent progress indicator allowed users to track exactly where they were in the process.
Preparation guidance
A “Before you begin” section told users the application would take about ten minutes and listed the documents required.
Contextual assistance
Information icons next to complex fields provided quick explanations without forcing users to leave the flow.
Formatting assistance
Fields automatically formatted inputs when possible, reducing cognitive load and preventing errors.
User testing confirmed these changes helped participants feel more comfortable progressing through the application.
6. Accessibility and inclusive design
Because Medicare applicants include older adults and individuals with varying technical abilities, accessibility was a critical consideration.
The redesigned experience followed Abyss accessibility guidelines, including:
keyboard-accessible help elements
descriptive field guidance
clear labels and instructions
accessible error messaging
These changes ensured the tool was usable for a broader range of applicants.
Results
The redesigned enrollment experience produced measurable improvements in both usability and business outcomes.
Improved completion rates
Simplifying the flow and increasing transparency helped reverse the decline in start-to-complete conversions.
Reduced application abandonment
Clear progress indicators and preparation guidance removed uncertainty that previously caused users to drop off.
Better mobile performance
Mobile-friendly layouts and simplified input flows improved usability for the growing number of mobile applicants.
Higher user confidence and satisfaction
User testing showed participants appreciated:
knowing what to prepare before starting
being able to track their progress
quick access to contextual explanations
These changes helped transform the enrollment experience from a confusing process into a guided journey that felt manageable and trustworthy.
✅ Impact at a glance
Increased enrollment completion rates
Reduced drop-off throughout the application process
Improved mobile usability
Greater user confidence during a complex healthcare decision
General Mills
Hello, Cereal Lovers
Challenge
By the early 2010s, traditional cold cereal was losing ground at breakfast to trendier and perceived healthier options like yogurt, smoothies, and oatmeal. Despite being present in the vast majority of American households, cereal consumption had been gradually declining as consumer habits shifted toward more portable or protein-focused morning foods.
General Mills set out to reignite excitement around cereal by reminding people why they loved it in the first place. The goal was to reposition cereal not just as a breakfast routine, but as a nostalgic, playful cultural staple worth celebrating again.
Approach
The Hello, Cereal Lovers campaign was created as a fully integrated brand initiative designed to reconnect consumers with the joy of cereal through storytelling, community engagement, and digital experiences.
The campaign launched with television spots and a dedicated website experience that served as a hub for cereal culture, recipes, and interactive content celebrating cereal in and beyond the breakfast bowl. Social channels, particularly Tumblr and other visual platforms, extended the experience by sharing playful content, fan contributions, and creative cereal mashups that encouraged people to participate and share their own cereal-inspired moments.
The tone leaned intentionally nostalgic and irreverent, treating cereal as a beloved cultural icon rather than a product to be hard-sold. Campaign messaging such as “Cerealously Fun” embraced the humor and personality of the category while keeping the brand voice light and memorable.
Results
What began as a campaign quickly grew into a social community celebrating cereal culture. The initiative generated strong engagement across social platforms, with hundreds of thousands of followers participating in the conversation and sharing cereal-inspired content.
Most importantly, the campaign helped reverse declining momentum for the category. During the campaign period, General Mills reported a 4% increase in cereal sales, demonstrating that celebrating nostalgia and community around a product could translate directly into renewed consumer demand.
The campaign also received industry recognition for its innovative use of social storytelling and integrated media, proving that even a decades-old category could find new life through a creative digital-first approach.
UnitedHealthcare Medicare Shopping / Online Enrollment
A bold reimagining of a timeless brand.
UnitedHealthcare Medicare Shopping / Online Enrollment
A bold reimagining of a timeless brand.